Life After Joint Intervention: A Comprehensive Overview
Hip surgery, a significant medical procedure, often becomes a necessary consideration for individuals experiencing chronic hip pain, limited mobility, or severe joint damage. Understanding the various aspects surrounding such an intervention—from initial considerations to the recovery journey—is crucial for anyone contemplating or preparing for this life-altering step. This article aims to provide a comprehensive overview, shedding light on the different types of procedures, the recovery process, and important factors to discuss with healthcare professionals.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Key Considerations Before Hip Surgery
Before undergoing any hip surgical procedure, individuals typically engage in thorough discussions with their healthcare team. These conversations often cover the underlying cause of hip pain, the extent of joint damage, and how daily life is affected. Factors such as age, overall health, activity level, and expectations for post-surgery outcomes play a significant role in determining suitability for surgery. Non-surgical treatments like physical therapy, medication, or injections are usually explored first. A decision for surgery is generally made when these conservative methods no longer provide adequate relief or when the joint damage is too severe.
Types of Hip Surgery Procedures
Hip surgery encompasses several different procedures, each designed to address specific conditions. Total hip replacement (arthroplasty) is one of the most common, involving the removal of damaged bone and cartilage and their replacement with prosthetic components. Hip resurfacing is an alternative where only the damaged surfaces of the femoral head and acetabulum are covered with metal implants, preserving more bone. Hip arthroscopy is a minimally invasive procedure used to diagnose and treat various hip problems, such as labral tears or impingement, using small incisions and specialized instruments. Other procedures include osteotomy, where bone is cut and reshaped to realign the joint, and fracture repair for hip fractures.
The Recovery Process Following Hip Surgery
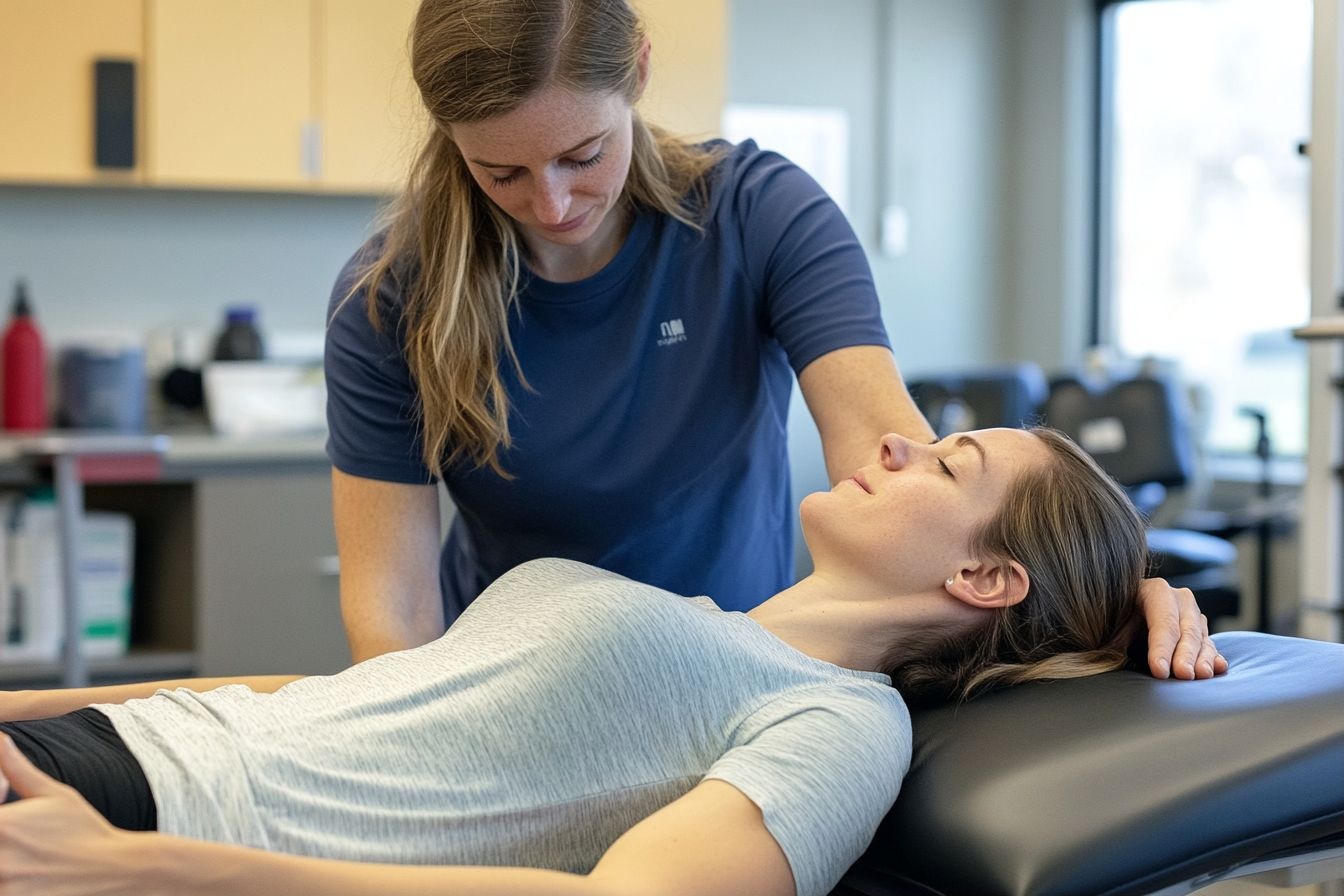
The recovery journey after hip surgery is a critical phase that requires commitment and patience. Immediately after surgery, patients typically begin physical therapy to restore strength and range of motion. The initial hospital stay can range from a few days to a week, depending on the type of surgery and individual progress. Post-discharge, rehabilitation often continues at home or in an outpatient setting, focusing on strengthening exercises, gait training, and learning how to safely perform daily activities. Full recovery can take several months, with consistent adherence to rehabilitation protocols being essential for optimal long-term results.
Potential Risks Associated with Hip Surgery
As with any surgical procedure, hip surgery carries certain risks, though serious complications are rare. Common risks include infection at the surgical site, blood clots (deep vein thrombosis), and adverse reactions to anesthesia. Other potential complications specific to hip surgery can include dislocation of the new joint, nerve damage, leg length discrepancy, and loosening or wear of the prosthetic components over time. Surgeons take extensive precautions to minimize these risks, and patients are typically educated on how to recognize and report any concerning symptoms during their recovery.
Expert Insights on Preparing for Hip Surgical Procedures
Preparing for hip surgery involves both physical and mental readiness. Healthcare professionals often advise patients to optimize their general health before surgery by addressing any existing medical conditions, maintaining a healthy weight, and stopping smoking. Pre-operative education sessions can help patients understand the procedure, what to expect during their hospital stay, and how to prepare their home for a safe recovery. This might include arranging for assistance, removing tripping hazards, and installing safety equipment like grab bars. Open communication with the surgical team and asking questions are encouraged to ensure a smooth experience.
Understanding the potential costs associated with hip surgery is an important consideration for many individuals. The overall expense can vary significantly based on the type of procedure, the specific hospital or surgical center, the surgeon’s fees, anesthesia costs, and the extent of post-operative care and rehabilitation required. For instance, a total hip replacement in the United States can range widely, influenced by geographical location and insurance coverage. Patients with health insurance plans typically have a portion of the costs covered, but out-of-pocket expenses such as deductibles, co-pays, and co-insurance can still be substantial. It’s advisable to consult with insurance providers and hospital billing departments to obtain a detailed estimate tailored to individual circumstances.
| Product/Service | Provider (Example) | Cost Estimation (USD) |
|---|---|---|
| Total Hip Replacement | Hospital Facilities | $30,000 - $100,000 |
| Hip Resurfacing | Specialized Clinics | $20,000 - $60,000 |
| Hip Arthroscopy (Minor) | Outpatient Centers | $5,000 - $15,000 |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Navigating the journey of hip surgery, from the initial decision-making to the extensive recovery period, requires careful planning and a clear understanding of the process. By being well-informed about the different types of procedures, potential risks, and the importance of rehabilitation, individuals can approach this significant medical intervention with greater confidence. Engaging proactively with healthcare providers and adhering to their guidance are key steps toward achieving a successful outcome and improved quality of life after joint intervention.




